Nuevas avenidas en el tratamiento quirúrgico de la epilepsia
Conferencia dada por el Doctor García de Sola en la Liga Española contra la Epilepsia, el pasado noviembre de 2012.
Jefe de Servicio del Hospital del Rosario
New avenues in surgical treatment of epilepsy
Email: rgsola@neurorgs.com
Introduction: Modern technological advances have been responsible for the new avenues for the surgical treatment of epilepsy developed during the last few years. Advances have influenced all aspects of surgical treatment, as shown below:
Patient selection and non-invasive assessment: a large range of non-invasive techniques presently exist to identify and characterise the epileptogenic zone. Modern structural neuroimaging has been crucial to improve the identification of epileptogenic lesions, allowing for the implementation of epilepsy surgery in less expert hands in a larger number of centres. Electroencephalography and video telemetry have become digital, allowing for considerable versatility and complex analysis, but still rely on human interpretation. Nuclear medicine techniques (SPECT and PET) have an important role to confirm finding and in patients with normal structural imaging. The reliability of functional neuroimaging to localise/lateralise function is still under considerable debate. The large number of clinical signs and symptoms presently described1 can aid in the non-invasive identification of the epileptogenic lobe, although their value is limited by the effects of seizure propagation to eloquent cortex and the fact that large cortical areas are functionally silent. Among our patients, scalp video telemetry is the method with the highest localising and predictive values compared to scalp EEG, MRI or SPECT2.
Invasive assessment: a variety of intracranial electrodes have become popular including foramen ovale, subtemporal strip, mat and depth electrodes. At Hospital La Princesa, we have obtained excellent results using foramen ovale electrodes for the assessment of temporal lobe epilepsy, which can be considered as a semi-invasive approach. We routinely use spike activation of etomidate in order to further characterise the epileptogenic zone3. Modern neuronavigation techniques can be very useful in localising the location of electrodes implanted during intraoperative acute electrocorticography. Pharmacological activation with etomidate can also aid in the evaluation of intraoperative electrocorticography. Electrical stimulation continues to be the gold standard for functional mapping, whereas evoked responses, functional neuroimaging, PET and MEG increasingly are emerging as complementary techniques. Over the last 10 years, invasive recordings have provided insight into the mechanisms of human epileptogenesis, in particular in the characterisation of neuronal synchronicity and network nodes, suggesting a reticular rather than purely focal onset for seizures. The use of acute electrocorticography to monitor the correct implantation of electrodes for chronic recordings is gaining acceptance.
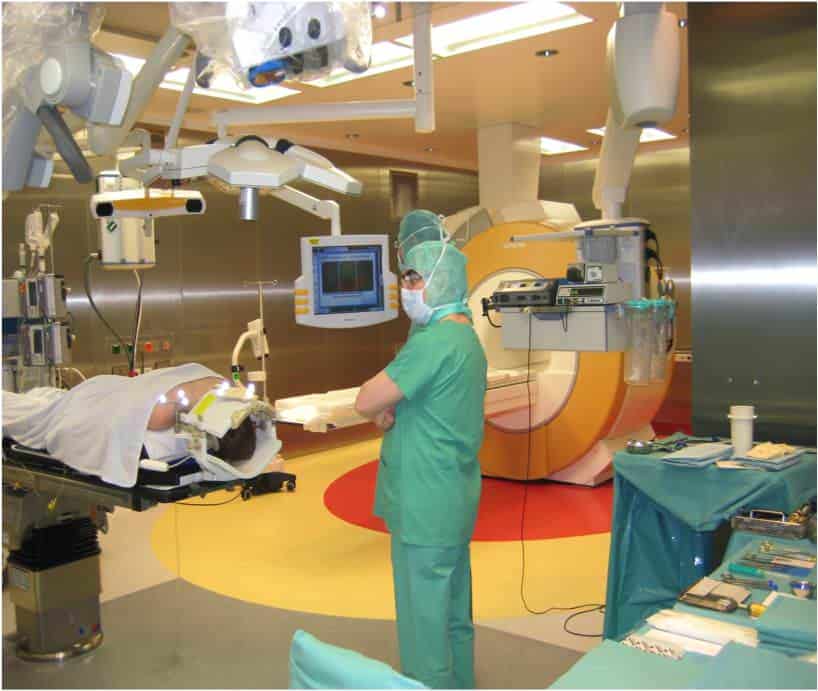
Surgical procedures: Modern advances in technology are re-designing the operating theatre for epilepsy surgery. At the Hospital de la Princesa the operating theatre has a microscope integrated with the neuronavigator, in additon to an annexed room to integrate neurophysiological studies and neuronavigator findings, culminating into an anatomo-functional map to guide resection. Otherwise, most surgical procedures themselves have not changed significantly in the last 10 years. Deep brain stimulation is emerging as an effective treatment of certain types of refractory epilepsy. The value of radiosurgery remains unclear.
Neuropathological studies: Neuropathological examination of resected specimens are crucial for the characterisation of epileptogenic lesions and their nature. Taxomony of some lesions, such as cortical dysplasia, has recently improved, which often results in higher prognostic accuracy. The main questions to be addressed by neuropathological studies are: What alterations in neuronal circuitry are necessary to generate an epileptogenic region? The most common lesion, hippocampal sclerosis, is characterized by a gliosis and neuronal loss which is most prominent in the CA1 field of the hippocampus, followed by the hilus, CA4 and CA3, whereas neurons in the dentate granular cell layer and, in particular, in the CA2 field are relatively spared.
Neuronal loss and gliosis and subsequent synaptic reorganization contribute to the establishment of recurrent seizures (chronic epilepsy). Seizure activity itself may produce further neuronal loss and gliosis in experimental models (chemical and electrophysiological) and in humans (patients without pre-existing epilepsy who develop status epilepticus). Yet, seizures may not be present in patients with severe damage of the hippocampal formation. An impairment of GABA-mediated inhibition is the main hypothesis to explain hyperexcitability of pyramidal cells and seizure activity:
- Inhibitory GABAergic inputs to pyramidal cells
- axo-dendritic cells or cells forming synapses only (or almost only) with dendrites
- axo-dendrosomatic cells or cells forming synapses with both the dendrites and somata, but with a preference for dendrites
- axo-somatodendritic cells or cells forming synapses with both the dendrites and somata, but with a preference for somata axo-axonic cells or cells forming synapses only with the initial axon initial segment (chandelier cells).
Microvascularization: The ubiquitous enzyme TNAP (tissue non-specific alkaline phosphatase) is found in numerous tissues such as liver, kidney and bone, but little attention has been paid to its expression and role in the brain. Observations in TNAP-KO mice, which analysed the role of this enzyme in osteogenesis, had suggested that TNAP might be involved in GABA neurotransmission. Our electron microscopic investigations suggest that alkaline phosphatase (AP) is found at the neuronal membranes and in synaptic contacts, it is proposed that the neuronal AP isoform (NAP), may be a key enzyme in regulating neurotransmission and could therefore play an important role in developmental plasticity and activity-dependent cortical functions. The subiculum is also emerging as an important factor in the genesis of temporal lobe epilepsy.
Post-surgical follow up: Modern technical advances appear to have been associated with better post-surgical results. In our centre, we have improved from 71% of patients enjoying Engel grades I-II (seizure free or almost seizure free) between 1990-2001 to 94% between 2001-2009.
Politics: over the last 10 years, awareness of epilepsy and its surgical treatment has significantly raised in the among the general public and political institutions but further work is necessary.
Future avenues: cellular and genetic therapies are emerging as future possibilities. The future role of optotherapy (excitation or inhibition of neuronal networks with light), ultrasound lesions, robotics, nanotechnology and nanorobotics remains unclear.
1Kellinghaus C, Lüders HO. The symptomatogenic zone. En: Textbook of Epilepsy Surgery. Ed: HO Lüders. Informa Healthcare, 2008.
2 Pastor J, Ortega GJ, Herrera-Peco I, Navas-García M, Navarrete EG, Alonso-Cerezo C, Pulido-Rivas P, Sola RG. Differential contribution of preoperatory studies to diagnosis in temporal lobe epilepsy surgery Rev Neurol. 2010 Oct 1;51(7):393-402.[Article in Spanish]
3Pastor J, Wix R, Meilán ML, Martínez-Chacón JL, de Dios E, Domínguez-Gadea L, Herrera-Peco I, Sola RG. Etomidate accurately localizes the epileptic area in patients with temporal lobe epilepsy. Epilepsia. 2010 Apr;51(4):602-9.
Video de la conferencia
[youtube id=»shOEZw1Bvqo» width=»100%»]